Mammograms, Diagnostic Testing, and Common Side Effects
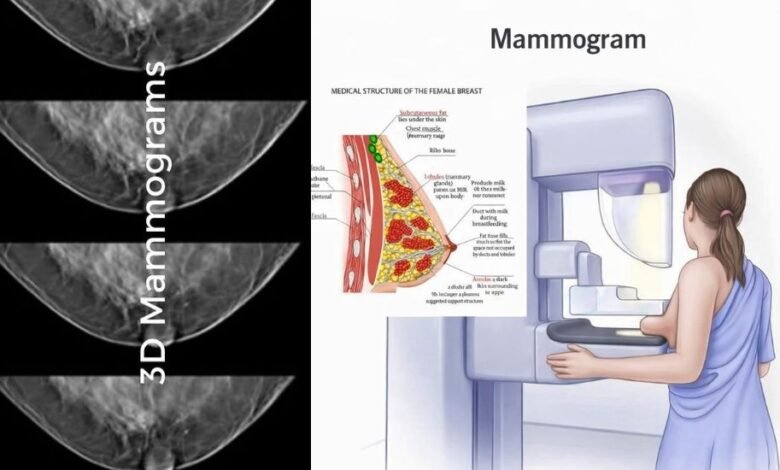
A mammogram is a specialized X-ray of the breast designed to detect changes in breast tissue that may not be visible or felt during a physical exam. The idea behind it is simple: catch potential problems early, when they are often easier to evaluate and manage. In practice, mammograms have become a routine part of preventive healthcare for many people, particularly as age and personal risk factors increase.
At its core, a mammogram works by compressing the breast between two flat surfaces and taking detailed X-ray images from different angles. This compression spreads out the breast tissue, making it easier to see small abnormalities such as masses or tiny calcium deposits. While the process can feel uncomfortable for a short time, it is typically quick and controlled by trained professionals who aim to balance image quality with patient comfort.
There are two main contexts in which mammograms are used. The first is routine screening, which is performed on people who have no noticeable symptoms. The goal here is early detection. The second is diagnostic use, which comes into play when something specific needs closer examination. This distinction matters, because it affects how the test is performed, how results are interpreted, and how patients experience the process.
Mammograms are not perfect tests. Like many tools in medicine, they work best when combined with other information, such as medical history, physical exams, and sometimes additional imaging. Still, they remain one of the most widely used methods for examining breast health and spotting changes that deserve further attention.
From a broader perspective, mammograms are part of a layered approach to healthcare. Rather than providing final answers on their own, they help narrow down questions. Think of them as a high-resolution snapshot that helps clinicians decide whether everything looks routine or whether more investigation is needed. That role is especially important when it comes to diagnostic mammograms.
Diagnostic Mammogram: How It Differs From Routine Screening
A diagnostic mammogram is not just a repeat of a standard screening mammogram. It is a more targeted, problem-solving exam designed to take a closer look at a specific area of concern. This concern might come from a previous screening result, a physical symptom, or a change noticed by the patient or healthcare provider.
Unlike routine screening, which usually involves a standard set of images, a diagnostic mammogram often includes additional views. These may involve magnification, focused compression, or different angles that allow the radiologist to examine a small area in greater detail. The process is more customized, adapting in real time based on what appears on the images.
One key difference is timing and interaction. During a diagnostic mammogram, images are often reviewed as they are taken. If something needs clarification, additional images can be captured during the same visit. This approach can reduce uncertainty and shorten the waiting period for next steps, which many people find reassuring.
Diagnostic mammograms are commonly ordered for several reasons, including:
-
A lump or thickening felt in the breast
-
Nipple discharge or skin changes
-
Pain localized to one area
-
An unusual finding on a routine screening mammogram
-
Follow-up after previous breast procedures or imaging
Because diagnostic mammograms focus on specific concerns, they can feel more intense emotionally. People often arrive with questions or anxiety about what prompted the exam. Clear communication and realistic expectations are important here. A diagnostic mammogram does not automatically mean something serious is wrong. In many cases, it simply confirms that a finding is harmless or related to normal tissue variations.
To use a simple comparison, a screening mammogram is like a wide-angle photo of a landscape, while a diagnostic mammogram is a zoomed-in shot of one particular area. Both images have value, but they serve different purposes. Together, they help create a clearer overall picture of breast health.
Mammogram Side Effects: What People Commonly Experience
When discussing mammogram side effects, it’s important to be clear and balanced. Mammograms are considered low-risk procedures, but that does not mean they are entirely free of temporary effects or concerns. Most side effects are mild, short-lived, and related to the mechanics of the test rather than long-term harm.
The most commonly reported side effect is discomfort or soreness during and shortly after the exam. This happens because breast tissue is compressed to obtain clear images. The sensation varies widely from person to person. Some describe it as pressure, others as pinching, and some barely notice it at all. Factors such as breast sensitivity, hormonal changes, and timing within the menstrual cycle can influence how the exam feels.
Another possible side effect is temporary breast tenderness following the mammogram. This usually resolves within hours or a day. Wearing a supportive bra and using mild pain relief, if appropriate, can help manage this discomfort. For most people, these effects are minor and do not interfere with daily activities.
Radiation exposure is another topic that often comes up when discussing mammogram side effects. Mammograms use low-dose radiation, and the amount is carefully regulated. The exposure from a single mammogram is generally considered minimal when weighed against the potential benefits of detecting changes early. That said, radiation exposure is cumulative over a lifetime, which is why screening schedules are designed thoughtfully rather than excessively.
False positives are a less physical but still meaningful side effect. A mammogram may identify something that looks suspicious but turns out to be benign after further testing. This can lead to additional imaging, biopsies, or short-term follow-ups. While these steps are taken out of caution, they can cause stress and anxiety for patients during the waiting period.
In rare cases, people may notice minor skin irritation from compression or positioning, particularly if they have sensitive skin or recent surgical scars. These effects are usually temporary and manageable.
Overall, mammogram side effects tend to be limited and short-term. Understanding what is normal and what to expect can make the experience less intimidating. When people feel informed, they are often better able to weigh temporary discomfort against the value of the information the test provides.
Benefits, Limitations, and Real-World Trade-Offs
Mammograms, including diagnostic mammograms, offer clear benefits, but they also come with limitations that deserve honest discussion. A balanced view helps people make informed decisions rather than relying on fear or unrealistic expectations.
One major benefit is early detection. Mammograms can identify changes in breast tissue before symptoms appear. This early insight allows healthcare providers to monitor changes, recommend follow-up tests, or rule out concerns. Diagnostic mammograms, in particular, help clarify ambiguous findings and reduce uncertainty when something unusual is spotted.
Another benefit is non-invasiveness. Compared to surgical procedures or biopsies, mammograms are relatively simple and quick. They provide valuable information without breaking the skin or requiring recovery time. For many people, this makes them an accessible first step when investigating breast concerns.
However, mammograms also have limitations. Dense breast tissue, for example, can make images harder to interpret. In such cases, abnormalities may be more difficult to distinguish from normal tissue. This does not mean mammograms are ineffective, but it does mean results must be interpreted carefully and sometimes supplemented with other imaging methods.
False negatives can occur as well. This means a mammogram may appear normal even though an issue exists. While this is less common, it highlights why mammograms are part of a broader diagnostic process rather than a standalone answer.
The emotional impact of mammogram results is another real-world trade-off. Waiting for results, undergoing follow-up tests, or receiving ambiguous findings can create stress. Even when outcomes are ultimately benign, the emotional experience can feel heavy in the moment. Open communication and realistic expectations can help reduce unnecessary worry.
To put it into everyday terms, a mammogram is similar to a detailed financial audit of one area of your life. It can highlight patterns, flag potential issues, and provide reassurance, but it does not predict the future with certainty. It offers information, not guarantees. That perspective can help keep expectations grounded and balanced.
Making Informed Choices and Preparing for a Mammogram
Preparing for a mammogram, whether routine or diagnostic, often starts with practical steps and clear communication. Simple choices can make the experience more comfortable and less stressful.
Many people find it helpful to schedule the exam at a time when their breasts are least sensitive. For those who experience hormonal changes, this might mean avoiding the days just before a menstrual period. Wearing a two-piece outfit can also make changing easier on the day of the appointment.
On the practical side, avoiding lotions, powders, or deodorants on the chest and underarms before the exam can prevent image artifacts that might look concerning on X-rays. Sharing prior imaging results or medical history with the imaging center can also improve accuracy and reduce unnecessary repeat tests.
Emotionally, it helps to approach the mammogram with realistic expectations. Feeling nervous is common, especially when undergoing a diagnostic mammogram. Asking questions, understanding why the test is being done, and knowing what the possible next steps might be can provide a sense of control.
In the broader context of health decisions, mammograms are just one part of an ongoing conversation. They do not define a person’s health on their own. Instead, they offer snapshots that help guide decisions over time. That long-term view is something Empire Magazines often emphasizes when discussing health topics: informed choices tend to come from context, not isolated results.
Ultimately, choosing to have a mammogram is about balancing information, comfort, and personal circumstances. For many, the reassurance gained from clear imaging outweighs the temporary discomfort or anxiety. For others, individualized screening schedules or additional discussions with healthcare providers may feel more appropriate.
Conclusion: Clear Perspective on Mammograms and Side Effects
Mammograms, including diagnostic mammograms, play an important role in modern healthcare by offering detailed insight into breast health. They are designed to detect changes early, clarify uncertain findings, and support informed medical decisions. While they are not without limitations or side effects, most effects are mild, temporary, and well understood.
Understanding the difference between routine screening and diagnostic mammograms helps set realistic expectations. Being aware of common mammogram side effects, from brief discomfort to emotional stress, allows people to approach the process with confidence rather than fear. When viewed as part of a broader healthcare strategy, mammograms become tools for clarity rather than sources of uncertainty.
The most valuable takeaway is balance. Mammograms provide useful information, but they work best when combined with medical guidance, personal history, and open communication. With that perspective, individuals can make choices that feel informed, measured, and right for their own situation.